- 5 May 2026
- The Neuro-Concept Blog
Prevent Rather Than Repair: Why Do We Talk About the Brain Too Late in Quebec?
In Quebec, we have learned to wait.
To wait for surgery.
To wait for a consultation.
To wait for a diagnosis.
But when it comes to brain health, waiting comes at an enormous cost — human, social, and economic. We usually talk about the brain only when it is “not working anymore,” too often once symptoms are established, persistent, and sometimes irreversible.
What if the real problem were not only a lack of resources, but our collective way of thinking about brain health?
A Brain in Distress… Within an Overwhelmed System
Neurological, cognitive, and functional disorders — concussions, mild traumatic brain injuries, chronic pain, concentration difficulties, cognitive fatigue, post-COVID symptoms — are on the rise. Yet Quebec’s public healthcare system remains largely organized around repair rather than prevention.
In practice, intervention often occurs only when:
- the person can no longer work,
- symptoms severely impair quality of life,
- the condition has become chronic,
- or multiple professionals have already been consulted without clear answers.
The result: an overloaded public system, endless waiting lists, and a deep sense of abandonment experienced by many patients. The brain — the central organ of human functioning — paradoxically becomes one of the most neglected upstream.

Why Is Brain Health Prevention the Poor Relative of the System?
Unlike cardiovascular health — where prevention, lifestyle habits, and screening are openly discussed — brain health remains surrounded by taboos and uncertainty. Several factors help explain this gap:
- Symptoms are often invisible: mental fatigue, sensory overload, and cognitive fog are not as easily measured as blood pressure.
- Training is fragmented: few integrated approaches exist between neurology, functional rehabilitation, kinesiology, psychophysiology, and applied neuroscience.
- Public funding prioritizes urgency: most investments are made once a situation becomes critical.
- A culture of endurance: in Quebec, we still too often value “pushing through” and “enduring” until exhaustion.
Frequent headaches, chronic cognitive fatigue, and attention difficulties are normalized… until the body and brain finally say stop.
Prevention: An Underused Lever

Preventing brain-related issues is neither a luxury nor “alternative” medicine. It means intervening early, when the brain is still highly plastic and responsive to adaptation. This includes:
- early assessment of cognitive and neuromotor functions,
- rapid management following a concussion or trauma,
- identifying neurological overload factors in the workplace,
- adjusting lifestyle and movement habits,
- individualized support before chronicity sets in.
Each early intervention can prevent months — even years — of consultations, fragmented therapies, work absences, and discouragement.
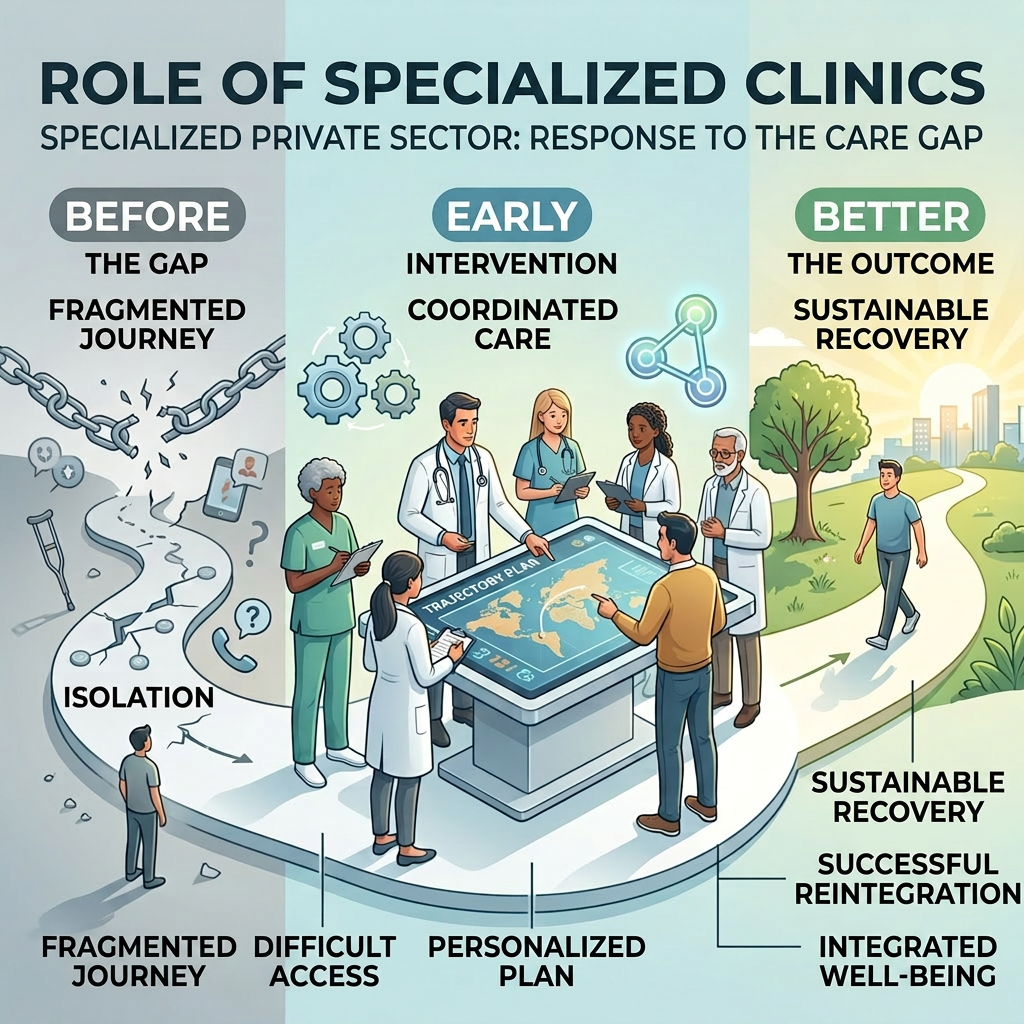
Specialized Private Care: An Imperfect but Essential Response
In this context, private clinics specializing in brain health are occupying an increasingly visible space. Their role is not to replace the public system, but to fill a structural gap.
These clinics often allow for:
- faster access to specialized expertise,
- in-depth, interdisciplinary assessments,
- personalized and continuous follow-up,
- interventions focused on function rather than diagnosis alone.
Criticized for their cost, they nevertheless raise an uncomfortable but essential question: is the real issue the existence of private care — or the lack of public prevention?
In a saturated system, the private sector sometimes becomes the only setting where prevention is still possible, before situations require heavy and costly public-system intervention.
Prevention and Equity: A False Dilemma?
Prevention and equity of access are often presented as opposites, as though early intervention only benefits a privileged few. Yet at a collective level, prevention is a powerful tool for equity:
- fewer prolonged work absences,
- less long-term disability,
- reduced pressure on emergency rooms and specialists,
- greater individual autonomy.
Ignoring brain health prevention means accepting that only the most severe — and most costly — cases will ultimately access public resources.
Rethinking Our Relationship With the Brain
Quebec is beginning to talk about mental health. It is beginning to talk about workplace well-being. But brain health remains confined to a late, fragmented, and often strictly biomedical vision.
Prevention means recognizing that the brain:
- becomes exhausted,
- becomes disorganized,
- adapts… or deteriorates,
depending on environment and how quickly intervention occurs.
Talking about the brain earlier is not about medicalizing everyday life. On the contrary, it helps avoid unnecessarily medicalizing situations that could have been addressed upstream.
What If Prevention Finally Became a Collective Priority?
As long as brain health is addressed too late, the public system will remain overloaded and patients will remain disoriented. Prevention is not an additional expense — it is a strategic investment.
Recognizing the complementary role of specialized private clinics, investing more in early assessment, and integrating prevention into public policies are concrete steps toward moving beyond a “repair at all costs” mindset.
Because when it comes to the brain, waiting always costs more than preventing.